Feeling connected in today’s world can be tough. Loneliness and social isolation are not unusual experiences.
It doesn’t matter whether you’re young, ageing, on a high income, impacted by the social determinants of health, living with multiple health conditions, going through a life transition or stuck like a hamster on a wheel.
We can all experience loneliness and social isolation. Unfortunately, it can profoundly impact our health and well-being, affect our individual quality of life, and contribute to the growing health and social care burden on our communities.
Instead of looking to yet another ‘magic pill’ to solve this challenge, we are seeing the rise of social prescribing to help reduce the demand for costly and sometimes ineffective medical interventions, prevent the escalation of social challenges, and promote a more holistic and person-centred approach to health and social care.
Social prescribing involves trusted referrers, such as doctors and other health or social care professionals, referring people to non-medical supports to improve their health and well-being, with the benefits broader than addressing social isolation and loneliness. Activities can include art, nature walks, gardening, music, sports, or volunteering and services such as counselling, financial or housing support.
The referral process can be as simple as pointing someone empowered to take control of their own life towards opportunities for support and increased connection. However, for people not ready to take that step alone, it involves connecting the individual to a link worker, who serves as a valuable resource and support while the person develops and implements their own personalised plan.
When I attended ASPIRE’s (Australian Social Prescribing Institute of Research and Education’s) International Social Prescribing Conference, I was impressed by the positive impact of the many grassroots social prescribing initiatives being driven by community organisations, health professionals, and volunteers.
However, I was struck more by what was missing!
Local efforts can only go so far towards addressing complex social issues when someone else in the system controls the levers and has the power to make decisions that either amplify or constrain those local efforts.

This challenge is not unique to social prescribing. It is typical of complex problems within interconnected systems where different stakeholders have differing levels of influence over interactions between parts of the bigger system.
This differing ability to pull the levers that influence systems is why connected stakeholder action is crucial to achieving positive system change.
Grassroots action is valuable. However, on its own, it can be like solving a jigsaw puzzle without seeing the full picture. You may connect some pieces by shape or colour, but many will remain disconnected or out of place. Important pieces might be overlooked, and wrong pieces might prevent the puzzle from being completed.
Adopting a systems thinking approach enables a focus on the whole puzzle and understanding how the pieces relate to each other and the bigger picture. You see patterns and themes that help organise the pieces into a coherent image. Systems thinking can help identify gaps and inconsistencies, refine the image, and improve the fit. It also allows you to discover new pieces or discard irrelevant ones, aiding in completing the puzzle.

However, the challenges that social prescribing aims to address require us to think and act systemically, i.e., use our understanding from systems thinking to guide actions and decisions.
The aim should be to identify the leverage points or places where a small change can have a big impact. If the authorising environment doesn’t provide the scope to pull the most impactful levers, then influencing and connecting who can is key.
So, how do you identify who you need to influence and connect?
Peter Checkland, one of the pioneers of systems thinking, also developed soft systems methodology (SSM) to understand and tackle complex problems involving people and social situations. SSM recognises that traditional methods don’t work well for these types of problems.
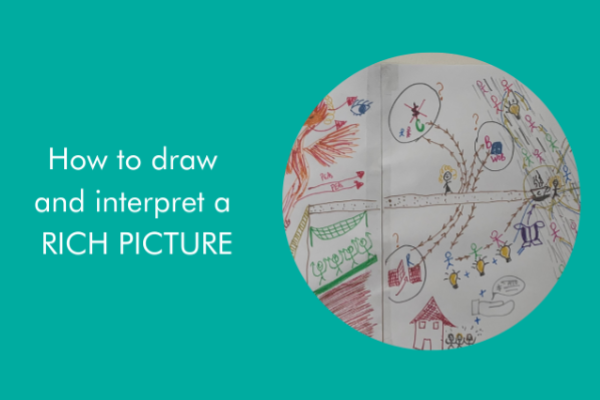
A great place to start with SSM is to draw what Checkland called a rich picture and interpret it using the pneumonic CATWOE. This visualisation and interpretation of a complex situation captures the main elements, actors, relationships, issues, and emotions involved. It helps us explore and communicate our understanding of the situation and identify opportunities and challenges for improvement.
As Peter Checkland said, “Pictures can be taken in as a whole and help to encourage holistic rather than reductionist thinking about a situation.”
If you want to learn more about drawing and interpreting a rich picture for your complex work or personal situation, this Free Mini-Course may be useful.
Social prescribing is constrained by the design of our health system, and many innovations are being driven by people and organisations that cannot influence health funding models.
Personally, I believe social prescribing and better connecting the health and social service systems deserve the attention of senior Government leaders who can drive connected, systemic change. However, it may be best to leave the topic of influencing systemic change for another newsletter.
If you’re also passionate about addressing systemic issues at the intersections of the health and community care systems, I’d love to chat, as I’m involved in some related projects.
